The retina is the light-sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. Any defect in layers of retina may lead to defective vision. In some cases, there may be small areas of the retina that are torn. These areas, called retinal tears or retinal breaks, can lead to retinal detachment.
What are the common problems of retina?
- Retinal Detachment
- ARMD – Age related macular degeneration.
- Retinal problems due to systemic diseases like diabetes, hypertension, auto-immune diseases, anemia, pregnancy
- Inflammatory diseases of retina
- Retinal Detachment
Retinal Detachment: Symptoms include a sudden or gradual increase in either the number of floaters, which are little “cobwebs” or specks that float about in your field of vision, and/or light flashes in the eye. Another symptom is the appearance of a curtain over the field of vision. A retinal detachment is a medical emergency. Anyone experiencing the symptoms of a retinal detachment should see an eye care professional immediately.
What are symptoms of diabetic retinopathy?
Blurring of vision due to bleeding & leakages of fluid from blood vessels in retina. In advanced diabetic retinopathy, formation of abnormal blood vessels on the retina, which may grow to vitreous also. These abnormal vessels are fragile and lead to bleeding which causes sudden and painless decrease in vision.
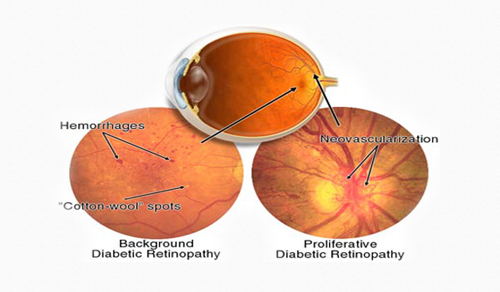
Different types of diabetic retinopathy:
Generally doctors classify diabetic retinopathy in two parts:
- Non-proliferative diabetic retinopathy (NPDR)
- Proliferative Diabetic Retinopathy (PDR)
PDR is the more damaging as it leads to many complications, which may be difficult to treat, like vitreous hemorrhage, neo-vascularization, glaucoma, secondary cataract, etc.
Who is most likely to get diabetic retinopathy?
Anyone who has diabetes for more than 10 years is vulnerable to diabetic retinopathy.
How can one prevent diabetic retinopathy?
A good control of sugar level can prolong the initiation of diabetic complications. Once detected, person has to be examined at regular intervals as suggested by doctors to prevent the permanent loss of vision.
Is diabetic retinopathy treatable?
Yes, in the initial phases with the help of lasers, we can prevent permanent loss to a great extent.
What are the available treatments for diabetic retinopathy?
- Laser
- Intra-Vitreal injection
- Surgery
How does LASER treatment work?
With the help of laser, treat unwanted blood vessels & tissue so that the healthy tissue can get proper supply of blood. This is done with the intention of stabilizing the vision. Improvement in vision may not always occur. One may have to repeat the laser treatment many times as per the diabetic retinopathy status.
Intra-Vitreal Injections: Latest treatment available for Diabetic Retinopathy, where intra-vitreal injection can help in resolving the vitreous hemorrhage and shrinking of neo-vascularization.
Surgery: It is a very complex operation, which may sometimes last for few hours. The surgeon removes unwanted tissue & laser the retina directly.
Can the patient get good vision after surgery?
In some cases, vision recovery is good, but depending on pre-existing diseases, vision recovery may vary.
What are the different types of retinal detachment?
There are three different types of retinal detachment:
- Rhegmatogenous: A tear or break in the retina allows fluid to get under the retina and separate it from the retinal pigment epithelium (RPE), the pigmented cell layer that nourishes the retina. These types of retinal detachments are the most common.
- Tractional: In this type of detachment, scar tissue on the retina’s surface contracts and causes the retina to separate from the RPE. This type of detachment is less common. It occurs secondary to problems like diabetic retinopathy and vein occlusions.
- Exudative: Frequently caused by retinal diseases, including inflammatory disorders and injury/trauma to the eye. In this type, fluid leaks into the area underneath the retina, but there are no tears or breaks in the retina.
Dr Shital

Dr. Shital S. Lalwani is an experienced ophthalmologist and general physician in Pune with over 21 years of experience. He practices at Jeevan Sparsh Eye Hospital Market Yard, Kondhawa, NIBM . Dr. Lalwani completed his MBBS in 2002 and DNB in Ophthalmology in 2006.